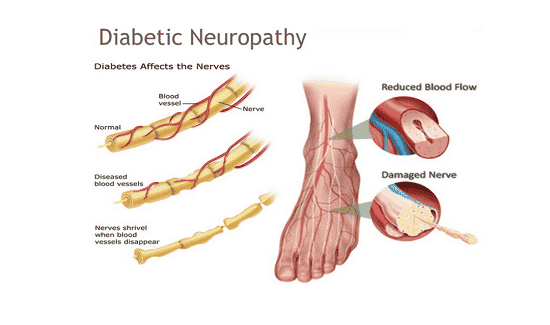
What is diabetic neuropathy?
Diabetic neuropathy is damage to the nerves caused by high blood sugar glucose. There are different types of diabetic neuropathy that can be defined both by the damage being caused and the symptoms experienced by patients. Diabetic neuropathy can take four different forms that are discussed in this article. The first of these is peripheral diabetic neuropathy.
Peripheral neuropathy
Damage to nerves at the bodily extremities such as the feet and legs is referred to as peripheral neuropathy. It is most common in the feet and legs but can also be experienced in the hands and arms. Up to 70% of people with diabetes will experience some form of peripheral neuropathy at some point. It is experienced in a number of ways but mainly as numbness in these areas.
Numbness caused by peripheral neuropathy
Damage to nerves caused by chronically high blood sugar levels reduces their ability to send signals to the brain and to other parts of the body. Nerve damage in these parts of the body therefore leads to a gradual loss of sensation, which can become permanent over time. It is the most common symptom of peripheral neuropathy and can develop gradually, making it difficult to detect. It is also often mistaken as an effect of aging. Treatment is simply the regulation of blood glucose.
Muscle weakness
High blood sugar levels can also damage the nerves responsible for telling muscles how and when to move. Gradually, these muscles become unused and therefore weaken. Typical symptoms of muscle weakness induced by diabetic peripheral neuropathy include:
- Difficulty getting in and out of chairs,
- Difficulty walking, and
- An inability to hold onto things by hand.
This can also lead to problems with self-balance and general coordination.
Inability to sense temperature changes
Nerves are also responsible for our ability to feel temperature. Therefore damage to the nerves can result in an inability to accurately sense hot or cold in parts of the body. Higher foot temperatures are common in sufferers of peripheral diabetic neuropathy, which can lead to other complications. For example, higher foot temperatures can result in ulcerations on the feet that can go undetected by patients.
Pain
Severe nerve damage at bodily peripheries can result in pain as well as numbness. Pain caused by peripheral neuropathy is most commonly treated with simple pain relief.
Autonomic neuropathy
Autonomic neuropathy is damage caused to nerves throughout the body rather than in a specific body part such as the arms, feet or legs. It can be caused by different conditions; however, diabetes is the most common cause. Autonomic neuropathy can also be differentiated from peripheral neuropathy by the damage being caused to nerves that control involuntary bodily functions rather than motor functions such as movement. Such involuntary bodily functions can include:
- Blood pressure
- Temperature control
- Digestion
- Bladder function, and
- Sexual function
Common symptoms of autonomic neuropathy
The autonomic nervous system includes the heart, blood vessels and sweat glands. Damage to the autonomic nervous system can therefore result in cardiac and other systemic problems. Symptoms vary, with sufferers often experiencing the following:
- Dizziness when standing
Dizziness from autonomic neuropathy is caused by a sudden drop in blood pressure due to the autonomic system failing to send the messages necessary to regulate blood supply to the brain.
- Urinary problems
Urinary problems caused by neuropathy are typically an inability urinate, incontinence and an inability to sense when the bladder is full. Such symptoms can also lead to frequent urinary tract infections and are often diagnosed by a doctor.
- Sexual difficulties
Another means to diagnosis this type of neuropathy is through patients reporting difficulties in sexual function. This may be the case for both men and women.
- Difficulty digesting food
This might include the feeling of being full after eating very little, loss of appetite, bloating or nausea, difficulty swallowing and heartburn. Such symptoms are caused by changes in digestive function caused by damage to the involuntary nervous system that controls human digestion.
Other symptoms of autonomic neuropathy
Other symptoms can include an abnormal sweat response such as sweating too much or sweating too little. This can result in difficulty regulating body temperature. Another symptom can be sluggish pupil reactions, which sufferers will experience as an ability to adjust to changes from dark to light and difficulty driving at night. An inability to exercise due to the heart rate remaining constant despite exertion is another symptom patients may experience.
Proximal neuropathy
Proximal diabetic neuropathy is damage caused to the nerves that supply the lower half of the body, specifically damage to the nerves of the lumbosacral plexus. It is also known as diabetic amyotrophy and is diagnosed through nerve tests such as electromyography (EMG).
The damage to these nerves can result in sudden pain in the hip, buttocks and thigh. Such pain can sometimes be severe. It can also lead to weakness in the legs making it difficult to stand from a seated position as well as a loss of the knee-jerk reaction. Muscle-wasting, loss of muscle tissue and general weight loss may also be experienced.
Typically, symptoms will become gradually worse before improving over a period of months or years. However, symptoms do not generally go away altogether. The advised treatment is regulation of blood sugar levels and treatment of pain. Exercise is also advised.
Mononeuropathy (focal neuropathy)
Mononeuropathy, as the name suggests, is damage caused to a single nerve. Depending on where the nerve sits, this can lead to loss of movement or sensation. It is most often caused by injury but can also be caused by systemic disorders such as diabetic neuropathy. A common form of diabetic mononeuropathy is carpal tunnel syndrome, which is damage caused to the nerves supplying the wrist and hands.
Summary
Diabetic neuropathy can take different forms and is diagnosed through nerve tests or through discussing symptoms with your doctor. Symptoms can often be difficult to identify due to the loss of sensation typical to the condition. Treatment is best approached through the long-term regulation of blood glucose and the management of pain or other symptoms in the shorter term.
—