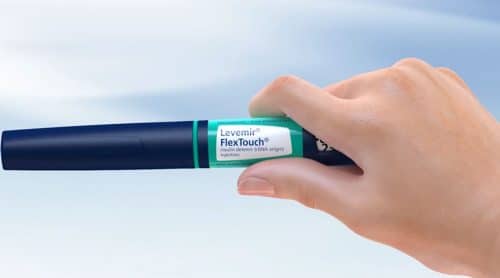
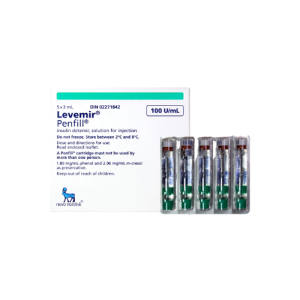
What is Levemir?
Levemir is a brand name of injectable insulin determir, used to manage blood sugar levels in people with diabetes. Leaving diabetes untreated can lead to health complications or even death. Most health complications that arise from untreated diabetes include kidney damage, blindness, loss of limbs, loss of sexual function and nerve problems. Controlling your blood sugar levels with this medication can reduce your risk for these symptoms, and it may also reduce your chance of having a heart attack or a stroke.
Insulin detemir is a synthetic form of insulin that releases a slow, steady amount of insulin in your body so that your cells can absorb sugar (glucose) and convert it into energy. It can be taken with or without other diabetes medications like metformin or exenatide.
What is the correct Levemir dosage?
The correct dose will depend on may factors, including the type of Levemir you are prescribed. You will likely need to inject the medication once or twice daily. If taken once, it should be taken with dinner or at bedtime. If taken twice a day, the second dosage should be given 12 hours after the morning dose. The injection sites should be rotated between the stomach, thigh, or back of the upper arm to avoid a skin condition called lipodystrophy.
In order to determine what dose of Levemir is right for you, your doctor or health care practitioner will monitor your blood glucose levels and consider many different factors. The amount of insulin you need will depend on many variables, such as stress, exercise, illness, the rate at which your body absorbs it, as well as any other medications taken or changes in your eating habits. You should never change or adjust your insulin dose without talking to your doctor first.
If this drug is used with a glucagon-like peptide (GLP)-1 receptor agonist, the injections should be given separately. A GLP-1 receptor agonist can be given in the same body area as Levemir, but do not inject them right next to each other.
If you have type 1 diabetes, you will need to take this medicine with a fast-acting insulin. Typically, your starting dosage will be one-third of your daily insulin requirements. The rest of the insulin needed should be made up of a fast-acting insulin to maintain blood sugar control during and after meals.
If you have type 2 diabetes, your starting dosage is likely to be 10 Units (or 0.1-0.2 Units/kg), which you will likely take in the evening, or it may be split into two daily doses. If you use a GLP-1 receptor agonist, the dose will likely be the same, taken once daily.
Later doses will be determined under the guidance of your doctor or health care provider, following routine glucose measurements.
Switching to Levemir from other insulin medications
If you have previously taken insulin glargine, you can convert to Levemir on a unit-for-unit basis.
If you have previously taken NPH insulin, you can also start taking this drug on a unit-for-unit basis; however, you may need to take more Levemir than NPH insulin.
Any time you switch forms of insulin, it is important that you keep a close eye on your glucose levels for the first few weeks. Your doctor or health care provider may need to adjust your dose and advise you when to take other diabetic medications.
How to use it?
Always make sure you read and understand the information leaflet before you take this medication. When you fill a prescription, it is important to check that there are no solid particles in the pen. Insulin detemir should be colorless and clear and kept at room temperature. Cold insulin can be painful if injected. Do not shake the pen, if you have it in pen form. When you are ready to inject the insulin, choose a patch of skin that is not red or itchy, as this may cause irritation or infection. Disinfect the injection site with rubbing alcohol and avoid injecting it directly into a vein or a muscle because it could cause low blood sugar. Do not rub the skin after the injection. Never mix Levemir with any other type of insulin, and never share your insulin pen, needle or vial, even if you have changed the needles. Doing so could cause a serious infection or transmission of diseases. Dispose of your used needles safely.
Try to take the medication at the same time each day, as a routine dosing schedule will allow this medication to work the best. If Levemir is not effective, or if you start to feel unwell (blood sugar too high or too low) while taking this form of insulin, tell your doctor right away.
Disclaimer: Please note that the contents of this community article are strictly for informational purposes and should not be considered as medical advice. This article, and other community articles, are not written or reviewed for medical validity by Canadian Insulin or its staff. All views and opinions expressed by the contributing authors are not endorsed by Canadian Insulin. Always consult a medical professional for medical advice, diagnosis, and treatment.